 Source: bing.com
Source: bing.comInsulin syringes, also known as diabetic syringes, are used to administer insulin to people with diabetes. Insulin is a hormone that helps regulate blood sugar levels, and it is necessary for people with diabetes to take insulin to keep their blood sugar levels under control. Insulin syringes are one of the most common ways for people to take insulin, and they come in a variety of sizes and types.
What is an Insulin Syringe?
 Source: bing.com
Source: bing.comAn insulin syringe is a medical instrument that is used to inject insulin into the body. It consists of several parts, including the barrel, plunger, and needle. The barrel is the long, cylindrical part of the syringe that holds the insulin. The plunger is the part of the syringe that is used to push the insulin out of the barrel and into the body. The needle is the small, thin part of the syringe that is inserted into the skin to deliver the insulin.
Types of Insulin Syringes
 Source: bing.com
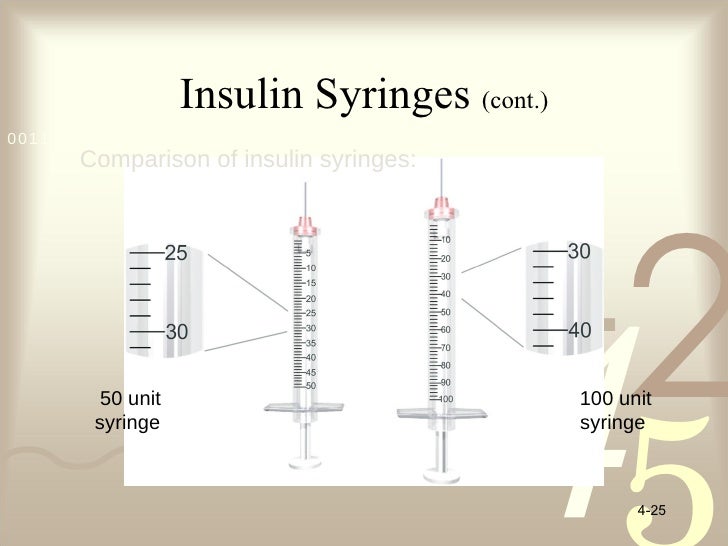
Source: bing.comThere are several types of insulin syringes available on the market. The most common types include U-100 syringes and U-40 syringes. U-100 syringes are used to administer insulin that has a concentration of 100 units per milliliter, while U-40 syringes are used to administer insulin that has a concentration of 40 units per milliliter. It is important to use the correct type of syringe for the concentration of insulin being administered.
Syringe Sizes
 Source: bing.com
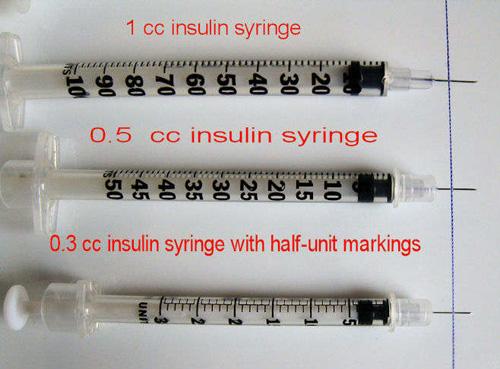
Source: bing.comInsulin syringes come in a variety of sizes, from 0.3 ml to 1 ml. The size of the syringe used depends on the amount of insulin being administered. Smaller doses of insulin require smaller syringes, while larger doses of insulin require larger syringes. It is important to use the correct size syringe to ensure the correct dosage of insulin is being administered.
How to Use an Insulin Syringe
 Source: bing.com
Source: bing.comUsing an insulin syringe is a simple process that involves a few steps. The first step is to wash your hands to ensure they are clean and free of any bacteria. Then, select the appropriate syringe size and type for the amount and concentration of insulin being administered. Remove the cap from the needle and draw the correct amount of insulin into the syringe. Next, clean the injection site with an alcohol swab and insert the needle into the skin at a 90-degree angle. Push the plunger down to inject the insulin, and then remove the needle from the skin. Dispose of the used needle and syringe in a sharps container.
Benefits of Insulin Syringes
 Source: bing.com
Source: bing.comInsulin syringes are a popular choice for administering insulin because they are easy to use, convenient, and cost-effective. They are also more accurate than other methods of insulin administration, such as insulin pens. Insulin syringes are available at most pharmacies and can be purchased without a prescription.
Drawbacks of Insulin Syringes
 Source: bing.com
Source: bing.comWhile insulin syringes have many benefits, there are also some drawbacks to using them. One of the biggest drawbacks is the need for multiple injections per day, which can be painful and inconvenient. Additionally, some people may have a fear of needles or a phobia of injections, which can make the use of insulin syringes difficult.
Conclusion
Insulin syringes are an important tool for people with diabetes who need to take insulin. They come in a variety of sizes and types and are easy to use and cost-effective. While there are some drawbacks to using insulin syringes, they are still one of the most common ways for people to take insulin and can help keep blood sugar levels under control.
 Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source:  Source:
Source: 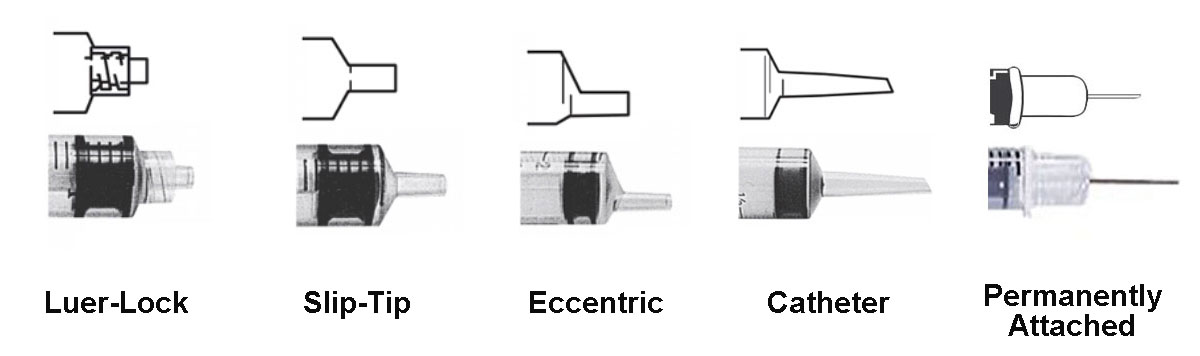 Source:
Source: 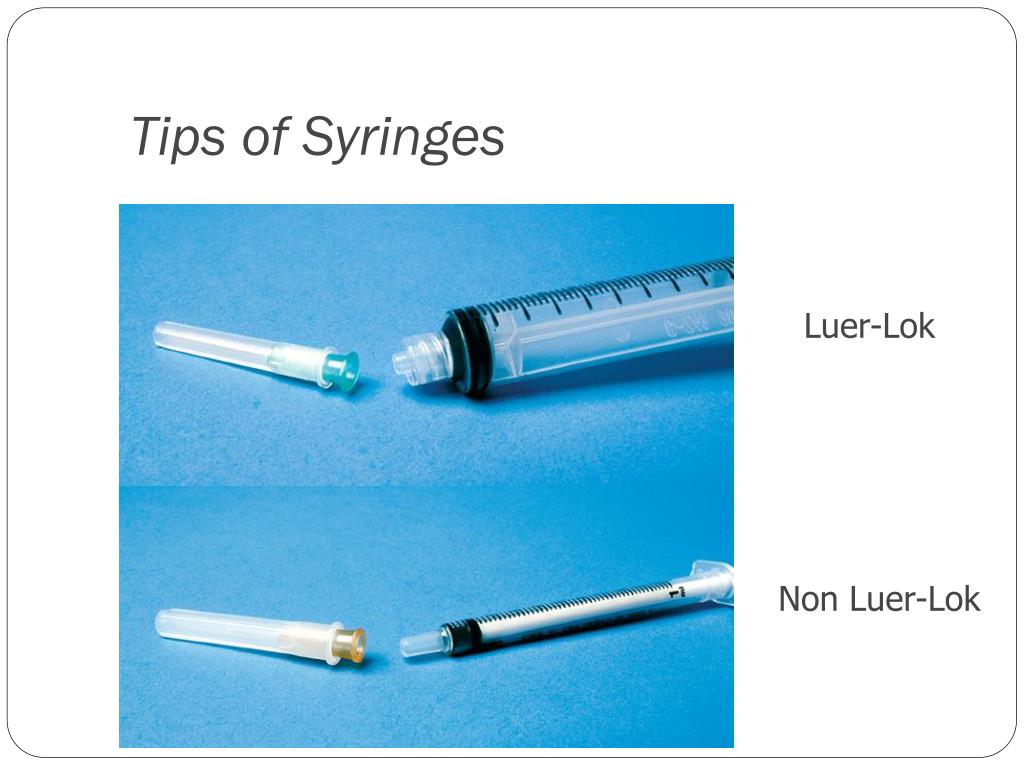 Source:
Source: